What is EPM?
EPM, or Equine Protozoal Myeloencephalitis, is a neurologic disease caused by the protozoan parasite Sarcocystis neurona. Although this disease has gained wide spread attention in recent years, it has actually been recognized as a disease in horses since 1964. It has been said that EPM occurs most commonly in Thoroughbreds, Standardbreds and Quarter Horses, and in horses aged 1-6, however, ANY breed of horse at ANY age can be diagnosed with EPM. The disease is also most common on the Eastern side of the United States, but can be found in horses on both coasts.
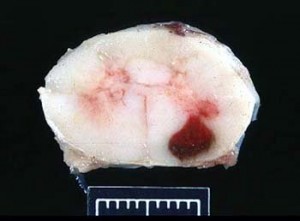
When the parasite migrates into the central nervous system, it causes necrosis (cell death) and bleeding in the spinal cord and brain, hence the name myelo-(spinal cord) -enceph- (brain) – alitis (inflammation of). Due to damage to the brain and spinal cord, horses that are suspected of having EPM tend to have neurologic signs such as wobbliness while walking. Unfortunately, this disease can cause a wide variety of clinical signs in horses, and is not easily diagnosed. It therefore presents a great challenge to veterinarians attempting to diagnose and treat horses with this disease.
How does a horse get EPM?
Horses are infected with EPM by ingesting the infective stage of the parasite, called the “sporocyst”. The parasite is passed in the feces of opossums onto areas where horses graze and into water sources. EPM CANNOT be transmitted between horses, so if your horse is around another horse with EPM, there is no evidence that your horse will be infected. Because horses are not able to pass the parasite to other horses, they are called a “dead-end host”. In addition, the majority of horses that are exposed to the parasite will develop a normal immune response and will not actually get the disease. Therefore it is likely that horses that do get EPM are under stress or are otherwise immunocompromised (have been ill recently or are chronically ill).
What are the clinical signs of EPM?
Horses that are suffering from EPM can unfortunately show a very wide variety of clinical signs. This is because the parasite can damage any part of the brain or spinal cord. Typical signs of EPM can include muscle wasting, especially of the hind end, ataxia (lack of coordination and weakness), and typically these signs are asymmetrical (on one side only). Veterinarians call this the “three A’s” (Ataxia, atrophy and asymmetry). However, EPM can look like almost every other neurologic disease! Some horses with EPM will show signs of circling and depression, while others will show signs of facial nerve paralysis (drooping of the ears, eyelid and muzzle on one side of the face). This is why often if your horse is showing signs of neurologic disease, your veterinarian will want to run diagnostic tests to rule out EPM.
How is EPM Diagnosed?
There are many different diagnostics available for EPM, some of which use blood, while others use cerebrospinal fluid (CSF) collected from the spinal canal. The decision about which diagnostics to use can be very different from veterinarian to veterinarian. These are two common diagnostic tests that veterinarians utilize:
- Blood Test: At Woodside Equine Clinic, if we have a patient that we suspect may have EPM, we generally start with a simple blood test that will show whether the horse has specific antigens (molecules that cause an immune response) that are specific to the parasite that causes EPM. These antigens will be present in the horse’s blood if the horse has been EXPOSED to the parasite. If the test is negative, it means that the horse has NOT been exposed to the parasite, and therefore it is unlikely that the horse has EPM. However, if the test is positive, it ONLY means that the horse has been exposed to the parasite. This does not, however, mean that the parasite has migrated to the central nervous system (brain and spinal cord) to cause EPM.
2) Cerebrospinal Fluid (CSF) Test: Some veterinarians choose to follow a blood test by looking for the same antigens to the parasite in the CSF. If the test on the CSF is positive, it is very likely that the parasite has migrated to the central nervous system, and the horse has EPM. In addition, if you have the results of both the blood and the CSF, it is very helpful to compare the two. In fact, some argue that by comparing the results of the blood and CSF tests, that you can most precisely diagnose EPM. However, obtaining CSF can be a fairly costly and sometimes invasive procedure, and therefore some veterinarians and owners choose to treat their horse based on blood results rather than performing a CSF test as well.
How is EPM treated?
There are 4 FDA approved medications for treatment of EPM, two of which I will discuss here, as they are the most commonly used methods. These treatments include a combination of Pyrimethamine and Sulfadiazine (brand name ReBalance), and ponazuril (brand name Marquis). Pyrimethamine-sulfa was the first treatment attempted for EPM, and was based on its effectiveness on other, similar parasites. Treatment with Pryimithemine-Sulfa can be very long, for up to 3-9 months orally. Success rate of this treatment is thought to be between 60% and 70%, however, many have reported that with this treatment there is a larger relapse rate after stopping treatment (around 10% relapse rate).
Ponazuril is a comparatively newer drug that was approved by the FDA in 2001, though it was in fact the first FDA approved drug for EPM. It is an oral paste that is given for at least 28 days, much shorter than the amount of time needed for treatment with Pyrimethamine-Sulfadiazine, although usually a loading dose (higher dose of medication at the beginning of treatment) is recommended. The efficacy rate of ponazuril is similar to that of Pyrimethamine-Sulfa, at 60-70%, though the relapse rate after stopping treatment is considered to be much lower (around 5% relapse rate). However, ponazuril is a more expensive treatment than Pyrimethamine-Sulfa. For both Pyrimethamine-Sulfa and ponazuril, treatment is more effective the earlier it is started in the disease process.
Many veterinarians will suggest one or even both of these medications based on the severity of clinical signs, and may even recommend other medications, such as DMSO (a potent ant-oxidant), which can help increase the amount of other medications that are absorbed into the central nervous system.
I hope that this clarifies some of the main principles of EPM, its diagnosis and treatment! If you have any questions about this article or your horse, please feel free to call Woodside Equine Clinic at (804) 798-3281.
For more information on EPM, please visit this very helpful website:
| EPM: Etiology, Diagnosis and Treatment |